Stroke Services
Strokes often occur without warning, and can happen to anyone.
Baptist's Brain & Spine Network offers a full range of stroke services to quickly treat and minimize the effects of a stroke with convenient locations throughout Eastern Arkansas, West Tennessee and North and Central Mississippi.
What is a stroke?
A stroke is a medical emergency that requires immediate care. It is in effect a brain attack and can happen to anyone at any age. And like a heart attack a stroke can be devastating, even fatal. Stroke is the fifth leading cause of death in the United States and a leading cause of disability in American adults.
A stroke occurs when blood flow to an area of the brain is either blocked by an obstruction or interrupted as a result of a ruptured blood vessel. When this happens, brain cells begin to die at a rate of 1.9 million cells per minute, and the subsequent brain damage often leads to disability or death.
Usually, the visible symptoms of a stroke come on suddenly and are only on one side of the body. And while stroke symptoms may not always seem like a medical emergency, you must act quickly.
B.E. F.A.S.T. When Strokes Occur
Stroke symptoms include slurring of speech, paralysis or numbing, problems seeing out of one or both eyes, disorientation, dizziness and headache. Every minute that passes can make a significant difference in the long-term prognosis of someone experiencing a stroke. However, quick action can reduce the impact of a stroke and reduce the damage to the brain. If you suspect someone is suffering a stroke, just remember to B.E. F.A.S.T.
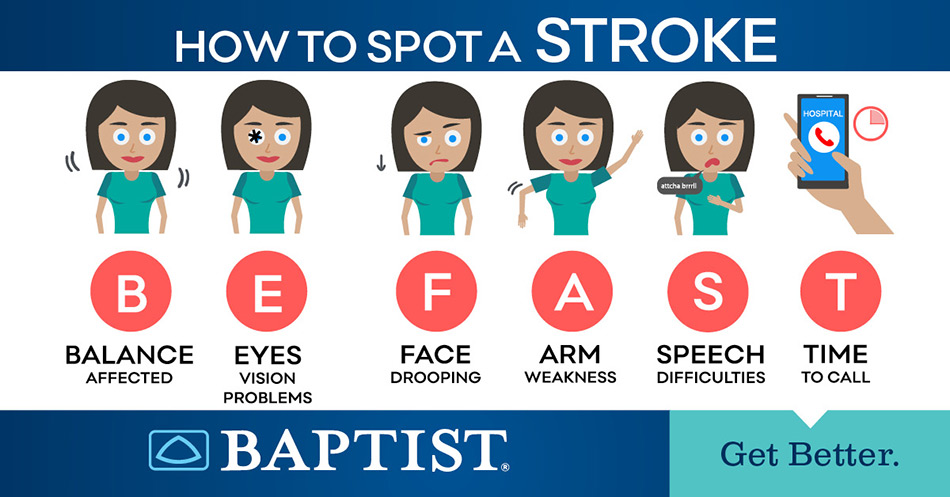
BALANCE: Is the potential stroke victim unsteady?
EYES: Do they have a vision problem in one or both eyes?
FACE: Ask the person to smile. Does one side droop?
ARMS: Ask the person to raise both arms. Does one side drift downward?
SPEECH: Ask the person to repeat a simple phrase. Is their speech slurred or strange?
TIME: If you observe any of these signs, call 9-1-1 immediately.
Other symptoms may include:
- Confusion
- Numbness, especially on one side of the body
- Difficulty with balance or walking in a straight line
- Severe headache for no reason
- Nausea and/or vomiting for no apparent reason
There are two kinds of strokes
An ischemic stroke is the most common type of stroke. It occurs when one of the blood vessels supplying the brain is narrowed or blocked by fatty deposits that build up in the blood vessels or by clots or other debris that lodge in the blood vessels in the brain.
A hemorrhagic stroke occurs when a blood vessel in the brain breaks or bursts and allows blood to leak into brain tissue, causing increased pressure in the head that may cause a severe headache in addition to the B.E. F.A.S.T. symptoms. This type of stroke is often associated with high blood pressure, excessive blood thinners, trauma or the result of an ischemic stroke.
Transient Ischemic Attacks
Often referred to as a ministroke, a transient ischemic attack, or TIA, is not an actual stroke, although its symptoms are very much like a stroke. It is a temporary (transient) disruption of blood supply to the brain due to a blockage or clot. A TIA is a warning sign that means you may have an increased risk for a full-blown ischemic stroke. If signs of a stroke occur and then pass, as often happens with a TIA, don’t ignore the symptoms and call 9-1-1. You will need a medical evaluation to understand why you had the temporary blockage of blood flow to the brain.
Are you at risk for a stroke?
Stroke may happen to anyone at any age. There are some risk factors for stroke you cannot control, such as your age, race or gender. However, there are a number of risk factors you can minimize with a change in lifestyle. These factors include:
High blood pressure
High blood pressure, or hypertension, is the leading cause of stroke. Fortunately, it is very manageable through a healthy diet, regular exercise, weight loss and medications. High blood pressure is known as the “silent killer” because you may not even be aware that you have it and the effects it can have on your health often go undetected until it’s too late. Have your blood pressure checked often, and talk to your doctor about what you can do to manage it.
Smoking, Vaping and Tobacco Use
Smoking cigarettes and electronic vapes and using other tobacco products increases your risk of having a stroke. Smoking exposes you to nicotine, carbon monoxide, and in the case of vapes, numerous other toxins and carcinogens that do damage to your cardiovascular system. For African Americans, the risk is more than twice as high. Quitting smoking of all forms and tobacco products usage is vital to your health, and there are many programs and plans to quit smoking available. Talk to your doctor about what smoking cessation options can work for you.
Diabetes
It is important to talk to your doctor about checking your blood sugar levels to find out if you may be at risk of having or developing diabetes. Diabetics may also have high blood pressure, which is another high risk factor for a stroke. Diabetics can live long, healthy lives, free from heart disease, stroke and other serious medical conditions by maintaining a heart-healthy diet, quitting smoking and vaping, maintaining a healthy weight and exercising daily.
Poor Diet
Eating a diet high in certain fats and sodium can lead to weight gain, high blood pressure and high cholesterol in the blood, all of which are high risk factors for developing a stroke. High cholesterol can also cause arterial disease, or clotting, decreasing blood flow to your heart and other organs, including your brain. Watch what you eat, and talk to your doctor or dietitian about ways you can improve your eating habits to feel and look better.
Atrial Fibrillation
Also known as AFib, atrial fibrillation is heart rhythm disorder that causes an irregular heartbeat in many people, increasing the chances of developing blood clots that can lead to a stroke. However, AFib is easily detected and treatable. A simple electrocardiogram, or ECG, or other diagnostic procedure may identify if you have AFib, and your doctor can tell you about available treatments to effectively manage or eliminate it.
How are strokes treated?
Treatment depends on the severity of the stroke and the condition of the patient and can range from emergency IV treatment to remove clots and restore blood flow, endovascular procedures including the insertion of a stent or the delivery of medicine directly to the brain or surgery to repair blood vessels and reduce pressure on the brain.
The stroke specialists at Baptist’s Brain & Spine Network work in collaboration with the neurologists and neurosurgeons from Semmes Murphey Clinic to diagnose and treat strokes quickly and minimize their impact so our patients have the best chance to fully recover and return to their normal lives as soon as possible.
As a Joint Commission-certified stroke center, we also offer our patients ample opportunities to be involved in multiple research trials.
How does Baptist diagnose and treat stroke emergencies?
When a patient arrives in our emergency department with neurological symptoms, our team will immediately assess their condition. We then use a telemedicine cart, a video communication technology called Teleneurology designed to allow a neurologist to provide 24/7 consultation from an off-site location.
The remote physician is on the video within minutes to help provide a diagnosis, oversee the administration of medicines, develop a plan of care and recommend transferring the patient to a higher level of care, if necessary.
This early intervention gives our patients the best possible chance for a better long-term recovery.
Our Stroke Specialists
Baptist’s team of neurology and neurosurgery specialists work together to diagnose and treat common to complex neurologic and neurosurgical problems related to stroke. Baptist’s four Stroke Centers have earned advanced certification to treat the most complex patients, and our Comprehensive Stroke Center in Memphis is certified by The Joint Commission as a leading clinical care and research facility that promotes leading-edge treatments and state-of-the-art equipment.
The multidisciplinary team works together using AI technology and system-wide communication platforms to ensure the patient receives the appropriate care. Patients can expect to receive exceptional care from a dedicated team that may include:
- Stroke medical director
- Neuro-critical care medical director
- Expert vascular neurologists
- Stroke nurses
- Stroke nurse practitioners
- Neuro-critical care unit and neuro step down unit
- Neuro radiology
- 24-hour stroke response team
- 24-hour neuro interventionist team
- Pharmacists
- Rehabilitation therapists
- Case managers
- Research trial facilitators
Stroke-ready facilities in the Mid-South
If you are experiencing any stroke related symptoms, please call 911 or visit your nearest emergency room.


